North America Back End Revenue Cycle Management Market Size & Forecast:
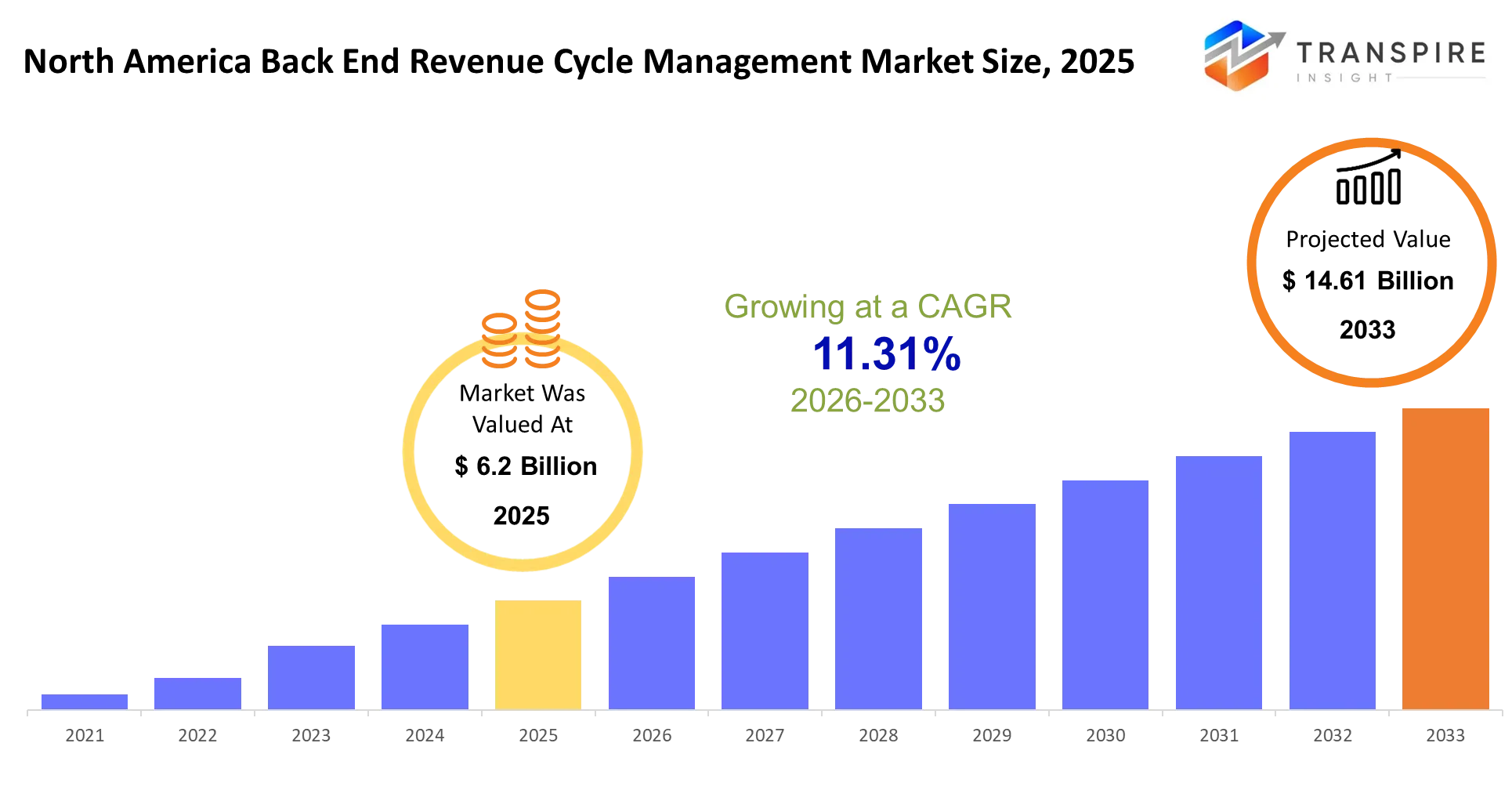
- North America Back End Revenue Cycle Management Market Size 2025: USD 6.2 Billion
- North America Back End Revenue Cycle Management Market Size 2033: USD 14.61 Billion
- North America Back End Revenue Cycle Management Market CAGR: 11.31%
- North America Back End Revenue Cycle Management Market Segments: By Type (Software, Services, Outsourcing, Consulting, Analytics, Others), By Application (Hospitals, Clinics, Physician Practices, Labs, Insurance, Others), By End-User (Healthcare Providers, Payers, Hospitals, Clinics, Others), By Deployment (Cloud, On-premises, Hybrid, SaaS, Platforms, Others).
To learn more about this report, Download Free Sample Report
North America Back End Revenue Cycle Management Market Summary:
The North America Back End Revenue Cycle Management Market size is estimated at USD 6.2 Billion in 2025 and is anticipated to reach USD 14.61 Billion by 2033, growing at a CAGR of 11.31% from 2026 to 2033. The North America Back End Revenue Cycle Management Market is experiencing steady growth as healthcare providers prioritize financial efficiency and compliance.
Back-end RCM solutions streamline critical processes which include medical coding and billing and claims management and denial resolution to help organizations decrease revenue loss. The rising healthcare costs together with intricate payer regulations lead providers throughout the United States and Canada to implement advanced RCM systems for improving accuracy and quickening reimbursements.
The North America Back End Revenue Cycle Management Market undergoes transformation through the adoption of automation and artificial intelligence and data analytics which enhance operational workflows while decreasing occurrences of manual mistakes. Hospitals and clinics and specialty care providers use these technologies to obtain current financial information which helps them improve their revenue results. The demand for efficient back-end RCM solutions will increase according to the growth of value-based care models which will lead to permanent market development.
What Has the Impact of Artificial Intelligence Been on the North America Back End Revenue Cycle Management Market?
The North American back-end revenue cycle management market now experiences fundamental changes because artificial intelligence drives the development of new technologies which help healthcare organizations handle their financial procedures through automated systems and data-based decision-making. The North American back end revenue cycle management market uses artificial intelligence to conduct comprehensive market analysis while enabling instant data assessment and operational analysis which detects billing patterns and claim denials and reimbursement patterns.
Providers achieve better demand forecasting through machine learning algorithms which help them identify upcoming demand more accurately while generating better revenue results that decrease operational waste. The new system enables hospitals and payers and third-party service providers to make better decisions which lead to improved financial results.
The North American back end revenue cycle management market uses artificial intelligence to develop intelligent automation systems which enhance claims processing and coding verification and denial management processes through efficient operational improvements. Automated workflows decrease human errors and speed up processing times and cut administrative expenses while they improve compliance with complicated regulations.
Healthcare organizations use AI-driven information to optimize their supply chains and manage costs which helps them remain profitable. The North American back end revenue cycle management market experiences a digital transformation trend that boosts AI adoption which provides organizations with a market edge and drives new developments while creating custom financial solutions.
Key Market Trends & Insights:
- The United States back end revenue cycle management market in North America reaches its peak through its 85% market share which will be maintained until 2025 because of its superior healthcare facilities.
- Canada stands out as the fastest expanding area which will achieve over 11% compound annual growth rate until 2030 because of its digital health technology investments.
- Medical billing services dominate the market with their 35% revenue share in 2025 which results from growing demand for outsourced services and needs to improve revenue streams.
- The second largest market segment belongs to coding and auditing services which gain advantages through mandatory compliance standards and demands for precise error elimination.
- The denial management sector represents the industry with the highest growth rate, which will achieve over 12% annual growth until 2030 because of increasing complexities in claim processes.
- Hospitals operate most of the applications which will reach 60% market share in 2025 because they treat numerous patients with sophisticated billing systems.
- The specialty clinic market segment experiences rapid growth because of rising outpatient services and the need for effective revenue cycle management solutions.
- Healthcare providers will achieve their advanced revenue cycle system implementation, which will allow them to maintain a market share above 65% for the year 2025.
- The third party RCM service providers represent the industry with the highest growth rate because companies adopt outsourcing while they seek cost reduction methods.
North America Back End Revenue Cycle Management Market Segmentation
By Type
The software will enable precise billing and coding along with efficient claim tracking. The services will manage daily operations to ensure uninterrupted workflow throughout healthcare facilities. The organization will benefit from outsourcing because it decreases internal tasks and enables financial management during periods of high claim activity. The combination of consulting services and analytics solutions will enable data assessment and performance evaluation to support superior decision-making.
Each type will add value in improving financial outcomes and reducing errors. The analytics tools will identify patterns that lead to denials and payment delays which require immediate response. The consulting support will assist organizations in meeting industry regulations while enhancing their operational processes. The organization will achieve effective financial management through the implementation of these various solutions.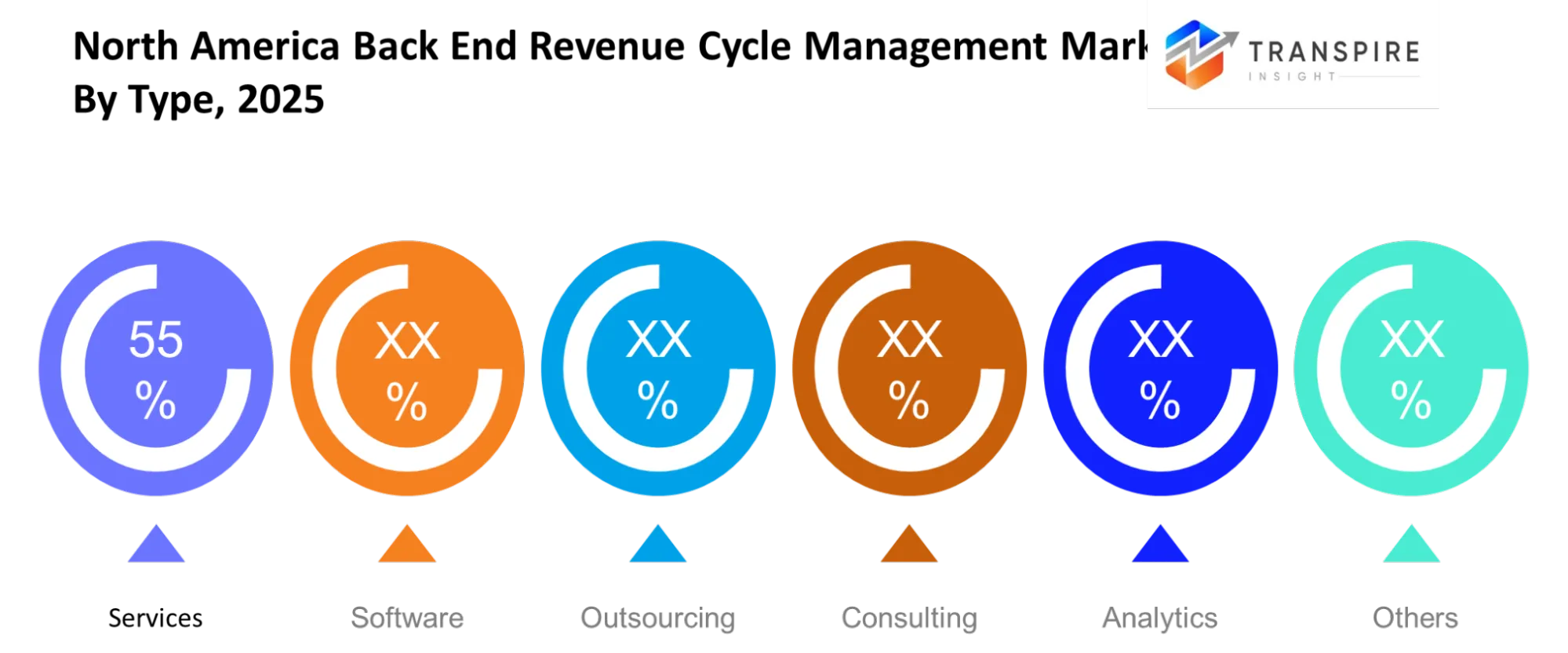
To learn more about this report, Download Free Sample Report
By Application
Hospitals will implement these systems because they need to handle their large patient volumes together with their complicated billing requirements. Clinics and physician practices will focus on simple and efficient billing processes. Labs need both precise claim management and prompt payment delivery. Insurance-related use will ensure better claim validation and faster approvals.
Different applications will show varied demand based on size and service type. Hospitals will need advanced systems for multi-level operations. Clinics and labs will choose budget-friendly solutions which they can use to perform their everyday activities. Insurance use will depend on strong data checks and smooth processing systems.
By End-User
The healthcare providers need effective billing systems for maintaining their revenue stream. The payers will utilize these tools for claim verification and reimbursement management. The hospitals and clinics will spend money to decrease delays while they work on increasing collection success. Each group will work toward achieving better financial understanding and faster operational procedures.
The end users want to decrease mistakes while they seek to speed up payment processing. Providers will use automation to increase accuracy and reduce manual effort. Payers will benefit from better data handling and fraud checks. Hospitals and clinics will work on improving patient billing experience and efficiency.
By Deployment
The expansion of cloud systems will happen because they provide flexibility and their updates are simple and their initial expenses are low. Organizations will continue to use on-premises installations because they need to maintain complete control over their data. Hybrid systems will use both security measures and access methods to achieve their desired equilibrium. SaaS and platform-based tools will create an environment that enables simple usage and delivers continuous product updates.
The organization will select its deployment method based on three factors which include its organizational size and its financial resources and its data requirements. Organizations will use cloud and SaaS solutions to establish their systems quickly while enabling employees to access their work from different locations. Organizations that use on-premises systems will gain complete authority to manage their confidential information. Hybrid solutions will assist organizations in digitally transforming their operations while maintaining their existing processes.
What are the Main Challenges for the North America Back End Revenue Cycle Management Market Growth?
The North America back end revenue cycle management market encounters significant technical difficulties and operational hindrances which create problems for productivity and system expansion. The system experiences performance limitations because of its complex billing systems and the need for ongoing coding updates and its difficulties in connecting with existing healthcare IT systems.
The process of handling numerous claims while maintaining precise results creates a situation which causes delays and increases the need for administrative tasks. The North America back end revenue cycle management market faces three main challenges which decrease process efficiency and create obstacles for automated work processes to function smoothly. The North America back end revenue cycle management market experiences market growth restrictions because of manufacturing and commercialization obstacles.
The need to comply with strict regulations which include data privacy legislation and healthcare requirements drives up both operational expenses and time needed for implementation. The need for extensive software development combined with specific customization requirements results in increased financial demands. The North America back end revenue cycle management market growth barriers create obstacles which prevent organizations from discovering new solutions.
The adoption process faces major obstacles because of two factors which include the shortage of qualified experts and the absence of proper infrastructure. Healthcare providers face implementation difficulties because they lack proper training and their staff members refuse to use digital technologies. Smaller clinics and organizations need funding to develop advanced systems but they face financial constraints which prevent them from acquiring such funding. The North America back end revenue cycle management market experiences market limitations which hinder organizations from achieving full adoption and better operational efficiency.
Country Insights
The United States will experience regional development because of its high healthcare expenditures combined with its sophisticated digital infrastructure and its widespread use of automated billing systems. Hospital networks that operate on a large scale will dedicate their resources toward developing accurate claim processing methods which will result in faster revenue collection. The need for effective back-end systems will increase because regulatory bodies continuously introduce new updates.
Canada will display consistent economic growth which the country will achieve through its healthcare system updates and its increasing dedication to digital recordkeeping. The government will enhance hospital and clinic IT adoption through its financial support for healthcare technology upgrades. Healthcare facilities of all sizes will implement budget-friendly solutions which enable them to handle billing and claims processing tasks in an efficient manner.
Mexico will display moderate economic growth because its healthcare system development and private sector funding will continue to advance. Healthcare centers in urban areas will adopt revenue optimization practices because they want to improve their operations. The full implementation of necessary systems will face obstacles from limited rural resources, but essential regions will continue to make steady advancements.
Recent Development News
In April 2026, U.S. RCM industry consolidation accelerates with a major $17B healthcare-adjacent acquisition: QXO’s acquisition of TopBuild reflects broader consolidation trends impacting healthcare-adjacent revenue-intensive industries, including outsourced financial operations and billing infrastructure. Such mega-deals reinforce capital flow into operational efficiency sectors closely linked to back-end RCM ecosystems.
Source: https://www.reuters.com
In February 2026, ACN Healthcare secured a ₹150 crore investment for RCM expansion: ACN Healthcare, a U.S.-linked revenue cycle management provider, received a significant growth investment aimed at expanding its healthcare billing and back-end RCM services. The funding will strengthen its operations across coding, billing automation, and denial management solutions in the U.S. healthcare system.
Source: https://economictimes.indiatimes.com
|
Report Metrics |
Details |
|
Market size value in 2025 |
USD 6.2 Billion |
|
Market size value in 2026 |
USD 6.9 Billion |
|
Revenue forecast in 2033 |
USD 14.61 Billion |
|
Growth rate |
CAGR of 11.31% from 2026 to 2033 |
|
Base year |
2025 |
|
Historical data |
2021 – 2024 |
|
Forecast period |
2026 – 2033 |
|
Report coverage |
Revenue forecast, competitive landscape, growth factors, and trends |
|
Country scope |
North America (Canada, The United States, and Mexico) |
|
Key company profiled |
Cerner, Epic Systems, McKesson, Change Healthcare, Optum, Allscripts, Athenahealth, Conifer Health, eClinicalWorks, NextGen Healthcare, R1 RCM, Kareo, Oracle, IBM, Cognizant |
|
Customization scope |
Free report customization (country, regional & segment scope). Avail customized purchase options to meet your exact research needs. |
|
Report Segmentation |
By Type (Software, Services, Outsourcing, Consulting, Analytics, Others), By Application (Hospitals, Clinics, Physician Practices, Labs, Insurance, Others), By End-User (Healthcare Providers, Payers, Hospitals, Clinics, Others), By Deployment (Cloud, On-premises, Hybrid, SaaS, Platforms, Others). |
How Can New Companies Establish a Strong Foothold in the North America Back End Revenue Cycle Management Market?
New market entrants in North America back-end revenue cycle management can create strong market positions by targeting specific market segments which currently have unmet requirements. Startups need to focus on denial management and coding accuracy and small-provider billing to establish their unique market position.
The North America back-end revenue cycle management market values solutions which directly decrease claim rejections and boost reimbursement processing times. Companies will acquire new clients more quickly when they present clear value propositions which show measurable results. The core of innovation will depend on AI-driven automation together with predictive analytics and cloud-based platform development.
North America back-end revenue cycle management market entrants should develop tools which can scale their operations while maintaining simple integration with current healthcare IT infrastructure. Smart automation technology helps organizations decrease their manual tasks while achieving better operational precision to solve major challenges faced in the industry. The dedication towards data security together with compliance measures will build stronger trust relationships between healthcare providers and the organization.
The company will achieve both market entry and credibility through strategic partnerships with hospitals and clinics and technology vendors. The company can enhance its market presence and solution compatibility through partnerships with electronic health record vendors and billing platform providers.
Key North America Back End Revenue Cycle Management Market Company Insights
The major players will sustain their market dominance through their advanced platform technology, extensive customer base, and ongoing development of their automation solutions. The companies will work to increase claim precision while they shorten their claim processing time and improve their data protection measures. The organization will achieve sustainable development through its investment in cloud-based systems together with its analytics capabilities.
Mid-sized firms will compete by offering flexible pricing models and specialized services tailored to hospitals and clinics. The company will establish a permanent customer base through its concentrated efforts in denial management together with its coding support services. The organization will expand its service capacity while increasing its market presence through collaborations with healthcare providers and technology vendors.
The new businesses will launch their operations through the introduction of disruptive products which use artificial intelligence and automation technology. The companies will concentrate on automating their billing tasks to achieve increased operational efficiency. The organization gains its competitive edge through its ability to implement solutions faster while offering user-friendly systems that adapt to new rules and business processes.
Company List
- Cerner
- Epic Systems
- McKesson
- Change Healthcare
- Optum
- Allscripts
- Athenahealth
- Conifer Health
- eClinicalWorks
- NextGen Healthcare
- R1 RCM
- Kareo
- Oracle
- IBM
- Cognizant
What are the Key Use-Cases Driving the Growth of the North America Back End Revenue Cycle Management Market?
The North America back end revenue cycle management market experiences steady growth because healthcare systems need better processes for handling claims and optimizing their revenue streams. Medical billing and coding through automated systems serves as a primary use case because advanced platforms minimize human mistakes while boosting accuracy in reimbursement processes. The healthcare systems use these systems, which enable hospitals and large networks to manage patient care at high levels while following intricate billing regulations.
Denial management and claims recovery systems serve as another essential use case for North America back end revenue cycle management solutions. Healthcare providers are increasingly adopting analytics-driven tools to identify patterns in claim rejections and take corrective action quickly. The process improves cash flow and decreases administrative expenses, which enables organizations to operate their business more effectively while growing their operations.
Outsourced revenue cycle services become essential when small and mid-sized healthcare organizations require them to help their market expansion. These organizations use third-party solutions to handle their back-end tasks because they want to avoid spending money on building their own operational systems. This use-case enables providers to deliver patient care while maintaining their financial operations and creates conditions for wider implementation.
The emergence of AI-based predictive analytics and workflow automation solutions provides organizations with improved decision-making tools that lead to better operational results. North America back end revenue cycle management market shows business expansion opportunities because organizations can achieve immediate insights and their operations capabilities. The market will experience continuous growth because digital healthcare adoption will drive demand for these adaptable solutions to meet future market requirements.
North America Back End Revenue Cycle Management Market Report Segmentation
By Type
- Software
- Services
- Outsourcing
- Consulting
- Analytics
- Others
By Application
- Hospitals
- Clinics
- Physician Practices
- Labs
- Insurance
- Others
By End-User
- Healthcare Providers
- Payers
- Hospitals
- Clinics
- Others
By Deployment
- Cloud
- On-premises
- Hybrid
- SaaS
- Platforms
- Others
Frequently Asked Questions
Find quick answers to common questions.
The Approximate North America Back End Revenue Cycle Management Market size for the Market will be USD 14.61 Billion in 2033.
The key Segments of the North America Back End Revenue Cycle Management Market are By Type (Software, Services, Outsourcing, Consulting, Analytics, Others), By Application (Hospitals, Clinics, Physician Practices, Labs, Insurance, Others), By End-User (Healthcare Providers, Payers, Hospitals, Clinics, Others), By Deployment (Cloud, On-premises, Hybrid, SaaS, Platforms, Others).
Major Players in the North America Back End Revenue Cycle Management Market are Cerner, Epic Systems, McKesson, Change Healthcare, Optum, Allscripts, Athenahealth, Conifer Health, eClinicalWorks, NextGen Healthcare, R1 RCM, Kareo, Oracle, IBM, Cognizant.
The Current Market size of the North America Back End Revenue Cycle Management Market is USD 6.2 Billion in 2025.
The North America Back End Revenue Cycle Management Market CAGR is 11.31%.
- Cerner
- Epic Systems
- McKesson
- Change Healthcare
- Optum
- Allscripts
- Athenahealth
- Conifer Health
- eClinicalWorks
- NextGen Healthcare
- R1 RCM
- Kareo
- Oracle
- IBM
- Cognizant
Recently Published Reports
-
Apr 2026
3D Optical Profiler Market
3D Optical Profiler Market Size, Share & Analysis Report By Type (Desktop 3D Optical Profiler, and Portable 3D Optical Profiler), By Technology (Confocal Technology, and White Light Interference), By End-Use Industry (Manufacturing, Research Institutions, Automotive, Aerospace and Defense, Medical Devices, and Other), and Geography (North America, Europe, Asia-Pacific, Middle East and Africa, South and Central America), 2021 - 2031
-
Apr 2026
Depth Sensor Market
Depth Sensor Market Size, Share & Analysis Report By Type (Infrared Depth Sensors, Time-of-Flight (ToF) Sensors, Stereo Vision Sensors, Structured Light Sensors, Ultrasonic Depth Sensors), By Application (Automotive, Robotics, Gaming, Consumer Electronics, Industrial Automation, Healthcare, Security & Surveillance, Others), By End Users (Automotive Manufacturers, Consumer Electronics Companies, Healthcare Providers, Industrial Companies, Security Agencies, Gaming Companies, Robotics Companies, Others), and Geography (North America, Europe, Asia-Pacific, Middle East and Africa, South and Central America), 2021 – 2031
-
Apr 2026
Digital Manufacturing Market
Digital Manufacturing Market Size, Share & Analysis Report By Component (Hardware, Software, and Services), By Technology (Robotics, 3D Printing, Internet of Things (IoT), and Others), By Application (Automotive and Transportation, Aerospace and Defense, Consumer Electronics, Industrial Machinery, and Others), By Process Type (Computer-Based Designing, Computer-Based Simulation, Computer 3D Visualization, Analytics, and Others), and Geography (North America, Europe, Asia-Pacific, Middle East and Africa, South and Central America), 2021 – 2031
-
Apr 2026
Digital Visa Services Market
Digital Visa Services Market Size, Share & Analysis Report By Type (Individual Travelers, Group Travelers), By Application (Tourism, Business Travel, Others), and Geography (North America, Europe, Asia-Pacific, Middle East and Africa, South and Central America), 2021 – 2031


